Regular exercise is beneficial for the general population; however, if your child has an eating disorder (ED), exercise can be dangerous. Participating in sports and frequent exercise with an existing ED can cause harm to your child’s body and even be deadly.
EDs are more common in athletes than non-athletes. EDs and disordered eating occur in up to 19% of male and 45% of female athletes. Furthermore, EDs are more prevalent in adolescent elite athletes than non-athletes, especially athletes who are female, 15-18 years old, and/or involved in high-risk sports, such as aesthetic, weight class, or endurance sports. Whether you consider your child an athlete or not, continuing to exercise with an ED can be destructive.
The information in this blog post particularly applies to exercise in anorexia nervosa and bulimia nervosa.
Heart Failure
EDs can lead to heart complications. About one-third of deaths in folks with anorexia nervosa are due to cardiac causes. Your child might develop an abnormal heart rate, including a decreased or increased heart rate. A slow heart rate is particularly common in folks with EDs. In adolescents, a slow heart rate is more common in those participating in team sports. Additionally, higher levels of exercise are associated with a slow heart rate in adolescents.
Your child may also experience low blood pressure. They may experience a rapid heartbeat or a drop in blood pressure when standing up, which can be dangerous. Symptoms of an abnormal heart rate and low blood pressure include fainting, dizziness, shortness of breath, and blurred vision. If your child’s heart rate or blood pressure decreases to a very low number, they may need to be hospitalized, and heart failure is more likely to occur.
Children with EDs also often experience a decrease in heart mass and structural changes to the heart. The image below illustrates how the heart can become smaller and change in structure in someone with anorexia nervosa.
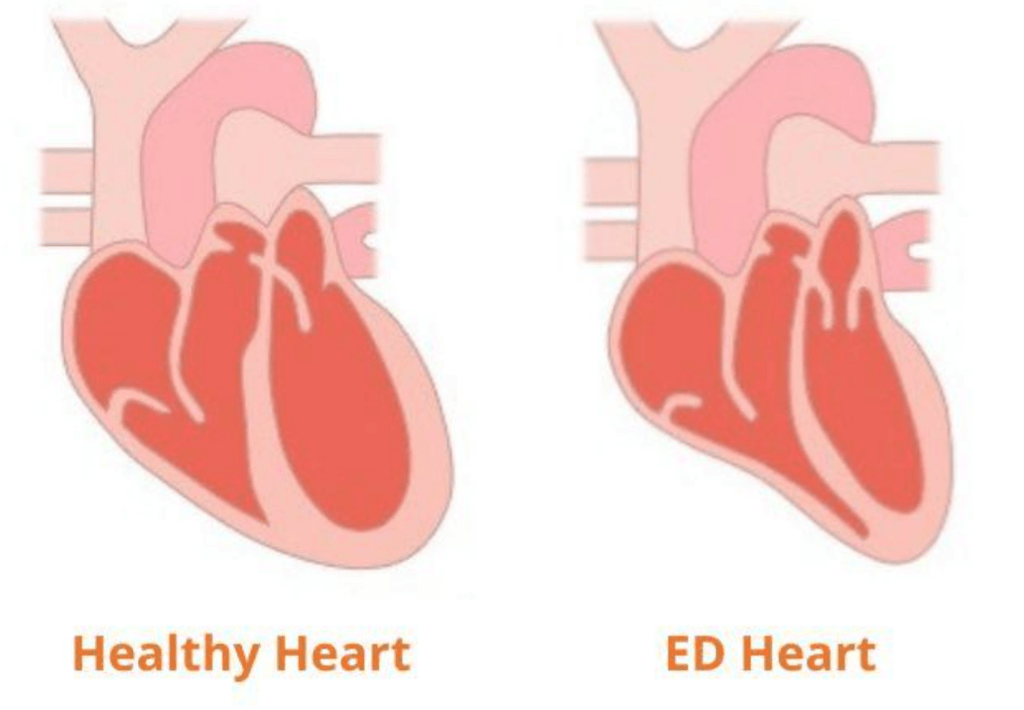
Continuing to exercise with an ED can be dangerous because it puts extra strain on a weak heart. Both an abnormal heart rate and low blood pressure can decrease the supply of oxygen and nutrient to organs like the brain. When we exercise, our hearts must work extra hard to meet our organs’ demand for oxygen. Overworking a heart that is not functioning the way it is supposed to can lead to heart failure. Furthermore, if your child is experiencing dizziness because not enough oxygen is getting to their brain, they may be more likely to faint and hurt themselves.
Electrolyte Imbalances
Electrolytes are minerals like potassium, sodium, phosphate, and magnesium that carry out important functions in our bodies. They are found in body fluids, like blood, and are necessary for muscle and nerve function. Often people with EDs have electrolyte imbalances, including low potassium, sodium, phosphate, and magnesium. Malnutrition, purging, excessive fluid intake, and refeeding syndrome can all lower electrolytes. Low levels of electrolytes may lead to muscle weakness, cramping, confusion, and in more severe cases an irregular heart rate, heart failure, or death.
Exercising with electrolyte imbalances can be dangerous. We lose electrolytes when we sweat, so exercising may further lower electrolyte levels. For healthy individuals, losing electrolytes when sweating will not cause harm, and electrolytes can be easily replaced by eating a snack or meal after exercise. For folks with EDs, losing electrolytes while exercising can increase the risk of heart failure because their electrolytes are typically low before they start exercising.
Dehydration
Folks living with EDs are at a higher risk of experiencing dehydration. Dehydration and overhydration can both lead to electrolyte imbalances, which can be harmful as described above. Additionally, when we are dehydrated, our bodies do not produce as much sweat. When our bodies do not sweat enough, our internal temperature can become too high. A high body temperature puts a strain on the cardiovascular system and heat illness may occur.6 Cramping, dizziness, nausea, weakness, or fainting may occur with a heat-related illness.
If your child has an ED and is dehydrated, exercising may make them even more dehydrated. Dehydration may lead to hospitalization. It is essential to limit exercise to reduce the risk of a heat-related illness, such as heat exhaustion or heat stroke. A heat stroke could lead to a seizure or coma.
Low Blood Sugars
Folks with EDs can have a low blood sugar level, which is known as hypoglycemia. If a child does not consume an adequate amount of carbohydrates, there are not enough blood sugars to provide their body with energy. EDs can cause liver damage as well, which impacts the body’s blood sugar levels as blood sugars are stored in the liver. The body breaks down muscles to provide the body with enough blood sugar for energy. Symptoms of hypoglycemia include headaches, confusion, weakness, dizziness, and potentially seizures or a coma.
Our bodies use lots of blood sugars when we exercise, which can make hypoglycemia worse. Hypoglycemia has a particular impact on the brain because the brain needs blood sugars to survive. If the brain does not get enough blood sugar, brain damage can occur.

Bone Fractures
While not necessarily deadly, EDs often negatively impact bone health and lead to low bone density. EDs can impact the body’s hormone levels, such as by increasing stress hormones and decreasing sex hormones. These hormones can decrease bone growth and increase bone loss. Furthermore, if your child normally has a period and their period becomes irregular or they miss it for six months, their bone health can become affected.
Exercising with low bone density can further contribute to poor bone health. Exercise can put a lot of pressure on already weak bones and increase the risk of bone fractures in your child. Bone fractures are even more likely to occur if your child is involved in contact sports. Long-term bone health can also be impacted as exercise can further disrupt hormone levels in the body.
How to Help Your Child
A first step towards recovery can be removing your child from sports. Exercising with an ED may increase your child’s risk of heart failure and lead to hospitalization. Limiting your child’s exercise can be essential for ED recovery.
Navigating ED recovery can be difficult, and we at Change Creates Change are here to help. You can book a free 15-minute consultation call with one of our clinicians today to discuss your child’s ED and exercise.
*Reserved for Canadian residents.


